Changing Faces, Changing Lives
Hamish’s Story

Hamish’s Mum Simone tells their story…
Hamish’s cranio story started the day he was born. No official diagnosis, just a comment from the Paediatrician about his odd head shape. At 3 weeks of age when leaving the hospital, they mentioned the possibility that he may have Craniosynostosis but that she would confirm at his 6 weeks check.
Hamish was 2 months old when he had his first CT scan and got the official diagnosis – Sagittal Craniosynostosis.
I immediately started researching everything I could. What would this mean for him? How would this impact his future? What was the best treatment option for Hamish? And what was the cause of this rare condition?
After doing a lot of research, we decided that we would go to Adelaide for his surgery. When Hamish (and his twin brother) were 4 months old, we all flew to Adelaide to meet the Surgeon for the first time.
After meeting Hamish’s Doctor, we discussed and accepted that the best option for Hamish was a full Cranial Vault Remodel (CVR). Hamish’s Sagittal suture was shown to be fused on the CT scan. His head was so big and heavy for him it was starting to impact his development. One example being he couldn’t lift his head during tummy time.
When Hamish’s surgery date was set for the 9th of October 2018, we prepared to move our family interstate for 3 weeks. Hamish’s grandparents also made the trip to provide support. The weeks leading up to surgery were extremely stressful, emotional and overwhelming. Aside from juggling the needs of twin babies, Hamish was also diagnosed with hip dysplasia which we needed to have treated prior to his CVR.
Whilst our anxiety levels were steadily on the rise throughout the week of the preoperative appointments, the day of surgery was the hardest part of the process by far. We first were dropped off to the hospital early to allow for Hamish to go through the necessary preoperative checks. The nurses we met during this period were comforting, friendly and supportive. The hardest two parts for us were having to hand Hamish to the doctors in theatre and then the 6 hour long wait. This 6 hours was the longest of our lives. It was an enormous relief to be back with Hamish in the Paediatric Intensive Care Unit (PICU) after the successful operation.


Hamish would go on to remain in hospital for a total of 5 days and then another 10 days as an outpatient.
Having spent the past 7 months avoiding crowds and illness, we celebrated our new sense of freedom by visiting Adelaide Zoo, taking many walks in the neighbourhood and having treats at the botanical gardens.
It wasn’t until after Hamish’s surgery that we first became aware of the wonderful team at Craniofacial Australia and were immediately welcomed in as if members of a new family. Hamish was gifted with a beautiful care package and upon hearing that Hamish’s twin would also require an unrelated surgery, the Foundation gifted him with a care package as well.
After returning to Canberra, it took a while for our family to adjust our lifestyle to ensure that Hamish stayed safe with part of his skull missing. As time passed, we didn’t think much about Hamish’s head and gradually let him enjoy all the activities that his friends took part in. We kept up with routine follow-up appointments in both Sydney and Adelaide and always made sure to incorporate a fun tourist activity. It was important for us to make Hamish feel like our trips were not solely medically related.
It was around the 2-year anniversary of Hamish’s surgery when we started to become concerned that Hamish’s skull bone had stopped growing. By 2021 a CT scan confirmed that Hamish’s bone growth had slowed significantly for reasons that no one could explain. With the hole in Hamish’s skull remaining stubbornly open and the doctors maintaining that there was still time for the cavity to close, we resigned to waiting and seeing what would happen.
A further two CT scans, one in 2023 and one in 2024, provided further evidence of very minimal bone growth. By this time Hamish had developed into a highly active child who enjoyed taking risks and aspired to play a variety of sports. It was therefore decided by his surgical team, that Hamish would benefit from an additional surgery in the form of a synthetic cranioplasty to cover his large (44mm x 96mm) bone deficit. A rib graft was initially recommended until the threat of them dissolving was deemed too high. Instead, the plan was for a custom 3D printed titanium plate be inserted into Hamish’s skull like a jigsaw puzzle piece.
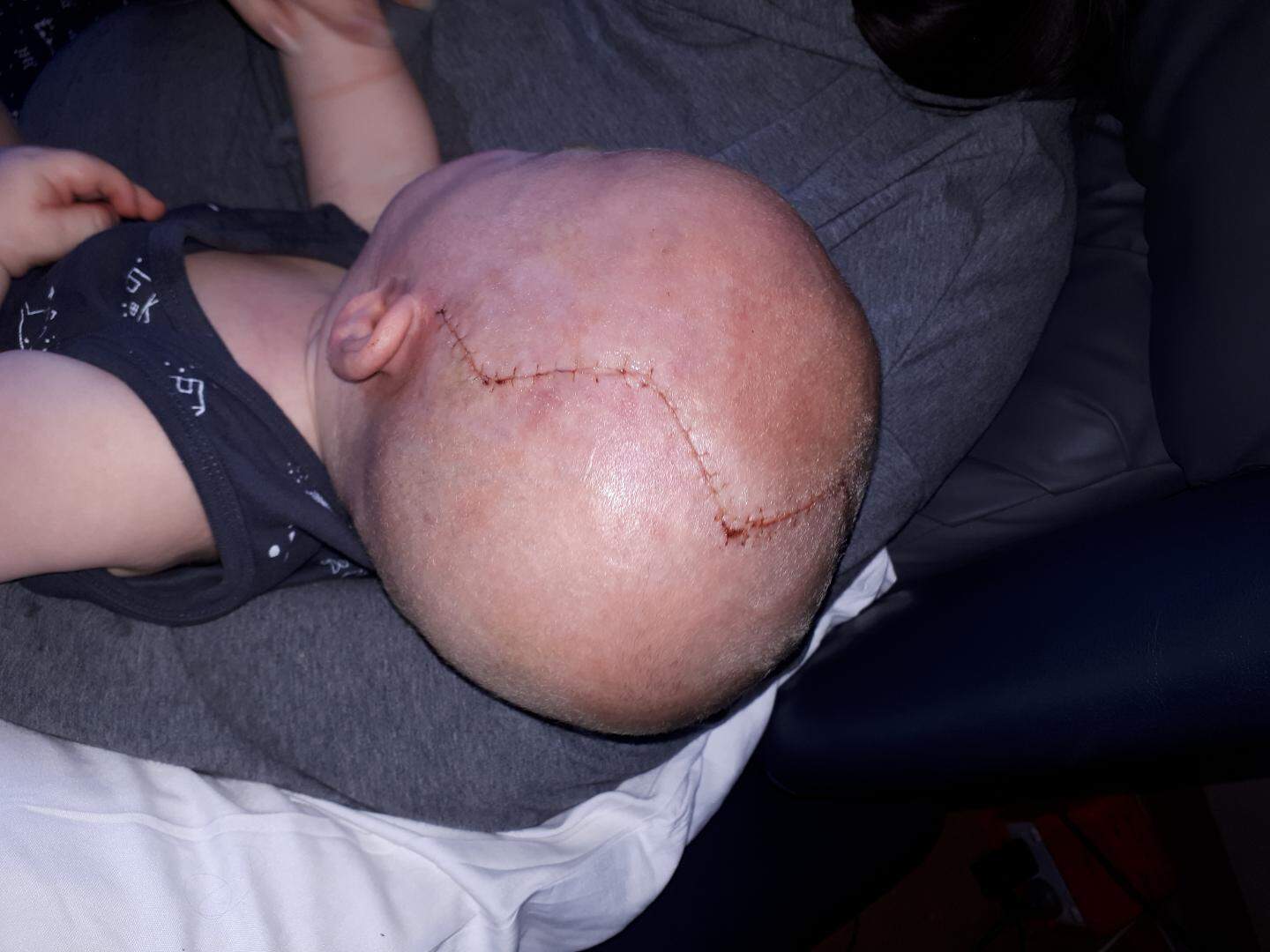

Almost 6 years after Hamish’s first surgery, he was again scheduled for cranial surgery, this time on the 24th of September 2024. The lead up to this second surgery was so much more difficult for everyone for a multitude of reasons. Firstly, Hamish had developed substantial trauma from his first operation and was now terrified of all kinds of hospital visits. Secondly, Hamish had grown self-conscious of having his hair shaved, having a visible scar and generally being different from his friends.
In an effort to normalise this for Hamish, we organised a “shave party” with his friends and family where everyone shaved their hair off. Hamish took part by shaving his Dad’s head with Hamish’s Mum getting a hair tattoo that resembled a zig-zag scar. We also approached Hamish’s school about having class discussions around individual differences and being inclusive of those with different appearances and experiences. We were also able to organise a school wide fund raiser (superheroes vs villains day) with the proceeds going to Craniofacial Australia.
And for ourselves as Hamish’s parents, we sought support from Claire the Family Support Coordinator at Craniofacial Australia as well as other Cranio Families.
So, we all packed up again and prepared for our next 3 week long stay in Adelaide. We spent the first week distracting ourselves by visiting a different beach every day around preoperative appointments. The second week included the surgery and the amazing team at Craniofacial Australia eased Hamish’s worries with a wonderful care package that gave him everything that he would need for his hospital stay.
Hamish’s second surgery was as smooth as one could hope for as everything went perfectly to plan without any complications and took far less time than anticipated. Hamish was able to go straight to the ward, avoiding any time in PICU, and was even discharged early due to his speedy recovery.
As an outpatient, we again spent the following 10 days in Adelaide doing as many enjoyable activities as possible. After 6 years, it finally felt like we could relax, stop worrying about getting ill and let Hamish dive “headfirst” into a “normal” childhood.
Hamish is currently loving participating in a variety of sports, playing with his friends and generally running amok. His high energy levels mean that he will never slow down (in fact he broke his wrist within months after his surgery) and leaves us with no doubt that we made the correct decision for Hamish by putting him through another surgery.